
Advantages for medical crew to be working on rotor-wing as well as on fixed-wing
Medical crew working on helicopters and aircraft missions
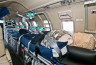
Air ambulance transfer flights are normally carried out under controlled conditions - however, as the patients are often intensive care patients, unexpected complications can occur at any time. Often this is an acutely worsening patient, and we can therefore speak of a risk collective.
Common critical problems
The most common complications are respiratory and ventilation problems - A and B problems (see note). Some of the patients who deteriorate in this way may suffer worsening respiratory function before departure due to stress and the hypoxic atmosphere at flight level. Others, who were extubated in hospital shortly before transport, may decompensate during the flight because they are muscularly not yet strong enough to compensate for the increased work of breathing in the hypoxic atmosphere of an aircraft.
In some patients, circulatory problems (C-problem) can occur due to bleeding or septic symptoms (although this is a rare complication as the patients have usually been cleared for transport after intensive medical examinations before departure). Where these problems occur, it makes it difficult for the medical staff to gain a routine in the diagnosis and therapy of the critically ill patient.
European Air Ambulance’s specialist nurses and doctors are not only deployed in ambulance aircraft, but also in the three rescue helicopters operated in Luxembourg and Germany by Luxembourg Air Rescue. The rescue systems in Luxembourg and Germany are designed as doctor-staffed rescue devices. In practice this means that the rescue helicopter is not only used to treat traumas, but also serves as a fast shuttle to take doctors and paramedics to the scene. The teams therefore treat a broad spectrum of patients, suffering a range of problems from the above-mentioned traumas to cardiac events such as acute coronary syndrome and neurological diseases.

Clinical and paramedical training
As a result, all EAA nurses must not only have clinical training but also be paramedics. Depending on which country they come from the training varies, but they all have in common a high level of competence in assisting in the treatment of acute pre-clinical settings. The same applies to the medical staff of LAR, who are not only specialists in anaesthesia and intensive medicine, but also all have an additional qualification as emergency physicians. By working regularly on the rescue helicopter, the doctors can maintain their skills in identifying and treating critically ill patients; and LAR nurses and doctors are trained in advanced life support as well as trauma management.
The advantages of the dual deployment can be summarised as follows:
- Double qualification of specialist nursing staff and physicians in clinically intensive medicine as well as pre-clinical medicine.
- Regular confrontation with critical patients.
- Routine care of patients with severe A, B, C, and D problems.
- Training in Advanced Life Support and Trauma Management.
Taken together, it means the crews are better able to react to any unexpected event during a secondary mission – which can only be good for the safety of all passengers entrusted to us.
Note:
In acute medicine, the following terms are used to quickly identify problems in critically ill patients:
- A-problem: Airway issues.
- B-Problem: Breathing, which involves lung function issues.
- C-Problem: Circulation, referring to circulatory problems of any type.
- D-Problem: Disability such as neurological deficit, stroke or paralysis.
- E-Problem: Environment/Exposure, reflecting exact consideration of accompanying circumstances.
