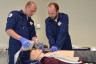
Medical training facility available to air ambulance crews
European Air Ambulance Medical Simulation and Training
The doctors and nurses who fly air ambulance missions must be prepared for any medical situation involving any patient – whether ill or injured, needing basic or intensive care, whether adult, child or new-born baby.
Training is vital for our lifesaving aeromedical teams, and Luxembourg Air Service (LAS), the parent company of European Air Ambulance (EAA), is committed to providing the very best ongoing training for all our medical staff.
At the heart of our headquarters is a new state-of-the-art SimCenter training facility, equipped with the latest medical simulation devices – an investment by LAS that ensures the teams flying our air ambulance missions are some of the best prepared anywhere in the world.
At the core of the SimCenter is the Simulator Room, where multiple different scenarios can be recreated thanks to 3D projectors, lighting and smoke effects – including road accidents, landscapes, or even a medical emergency in a hospital room.
Medical simulator mannequins are used within the scenarios, including the Sim Man 3G ® (Laerdal) – a high-end, full-scale adult patient simulator, which displays a whole range of symptoms and reactions and provides an extremely realistic training tool. Because the Sim Man is completely wireless, it can also be integrated into other training situations – including on our aircraft, helicopters, or at the onsite medical facility.
An infant version of the mannequin - a Sim Baby® (Laerdal) - is also used, and provides incredibly realistic training in emergency paediatric treatment and care.
As well as the patient simulators, LAA has invested in an Airway Trainer with a Video Laryngoscope (C-Mac ®) permanently available within the SimCenter, which can be connected via HDMI to a video screen ensuring all those involved in the training session get a clear view and can learn - whether or not they are actually performing the procedure themselves.
There is also a Basic Life Support trainer; a difficult airway trainer; and an EZ-IO ® drill along with artificial bones for practising intraosseous access, which can be a life-saving route to administer medicine.
Next to the simulator room is a debriefing room, with video capability.
Video debriefings focus on CRM (Crew Resource Management) aspects, and LAA sent a team of four doctors and four nurses to ‘train the trainer’ courses (EuroSim ® for the French speakers and InFact ® for the German-speakers).
This eight-strong team is now responsible for training, and for maintaining the exceptionally high standards expected at the SimCenter. External specialists are also invited to lead sessions according to their particular areas of expertise.
The LAA system follows the “train as you fight” principle, which is a common medical training method, and we work with different modules:
- Theoretical: Lectures on particular themes, for example paediatric themes presented by our neonatologist. We also use lecture-based education principles to introduce modifications/changes in guidelines. As LAA is an international air ambulance service, based in the heart of Europe in Luxembourg, we operate strictly according to European guidelines including those of the European Resuscitation Council (ERC ®) and the European Society of Cardiology (ESC ®) and in line with the European Trauma Guideline. If European guidelines are not available, we operate in line with recommendations of the French, German or English medical authorities.
- Practical: We train in mixed teams of doctors and nurses, using the mannequins for repetitive training to ensure medical staff react automatically and instinctively in critical situations.
- Skill training: We train in multiple skills, including airways, life support and defibrillation.
- Full-scale simulator: This is a tool to debrief on interactions within the team – to deal with human factors, which can have a big effect on the progress of a mission.
- Realistic environment training: We have a hangar directly beside the facility, which allows us to put the training equipment into our aircraft to practise in a real environment. This is a very important tool, allowing us to properly assess whether our emergency concept works in the aircraft/helicopter, or needs to be adapted.
LAA provides some of the very best aeromedical training available, and as well as standard in-house training, all staff must take part in sessions in the SimCenter. Staff are ERC ALS ®, PHTLS ® or TraumaManagement ® certified.
Doctors must complete a minimum of 25 endotracheal intubations per year and be certified as such; and thanks to close working relationships with nearby hospitals, our doctors can maintain their skills by working in local operating theatres.
All the evidence shows that regular training improves the performance of a team, and contributes to a lower rate of medical complications.
It’s also clear that by standardising training and introducing an enjoyable and low-stress atmosphere for all our teams, we see not only better behaviour and performance, but also a greater understanding and application of guidelines; improved efficiency; and ultimately better outcomes for our patients and cost savings for our clients.